It was my second voyage as a volunteer fistula surgeon to the landlocked desert country of Niger. The flight to Niger takes 5 hours from Charles De Gaulle airport in Paris, a labrynthe of terminals connected by shuttle buses. And here the tribal excursion begins, standing on line, all of us united beyond the limits of language and culture as one group complains in narcissistic theatricality, another crew sniffs and pouts in feigned, sullen indifference, another in stoic silence and another in cadenced soft murmurs looking from prayer compass to clock. The flight is 5 hours of time and 200 years back in economic development, to a place where life has little to do with nuance and luxury, and everything to do with survival and resilience. In the capital city of Niamey, airport porters battle with jobless locals to control the baggage from claim area to bus. Children with one hand, men with one leg and people crawling to and fro on polio twisted limbs are sprinkled throughout the crowd, scouring for hand-outs or the opportunity to work. If there is anything palpable on the way from the plane to the bus it is the bleak absence of opportunity.


The topography of Niger is… dusty. A landlocked desert relieved only by the Niger River coursing through the southernmost terrain, Niger is ranked last on the United Nations Development Fund index of human development (CIA-The World FactBook Dec 2006). Literacy rates for men are 21% and about 7% for women. Average life expectancy is 42 years of age. Medical colleagues born and raised in Niger command salaries of 100-300 USD per month. It is a place of want.

The National Hospital of Niamey, Niger
 The hospital is a former military installation built for quarantine in a network of single story low, flat-topped buildings connected by covered walkways and cement courtyards.
The hospital is a former military installation built for quarantine in a network of single story low, flat-topped buildings connected by covered walkways and cement courtyards.  Winding through the access road to the surgery building, women wrapped in Kinte cloth and long tunics and men in flowing robes and Tuareg turbans mill about in the universal comings and goings of people seeking and rendering healing. Outside, ubiquitous wood smoke spices the air, inside the low slung building the faint odor of disinfectant mixes with the dry heat. The operating rooms are doubled up with OR tables .
Winding through the access road to the surgery building, women wrapped in Kinte cloth and long tunics and men in flowing robes and Tuareg turbans mill about in the universal comings and goings of people seeking and rendering healing. Outside, ubiquitous wood smoke spices the air, inside the low slung building the faint odor of disinfectant mixes with the dry heat. The operating rooms are doubled up with OR tables .
The fistula women are waiting to be seen, having camped out in the “fistula courtyard” for days or weeks, arriving from the remotest areas of Niger and the surrounding countries of Benin, Nigeria, Burkina Faso and Mali. For some, an entire year’s earnings fund the journey to this hospital. The surgery building has a sunken courtyard on one side, and after traversing the cool tiled hallways, you emerge on the courtyard cat walk to see dozens of women and their children living, some for months, others for years, in a “sisterhood of suffering". Naked foam rubber mats, rinsed out daily with a garden hose lay flat in the sun to dry, ready for another night of urine-soaked sleep. The women are immaculate and enterprising, making beaded jewelry and learning to sew on machines donated by the International Organization for Women and Development (IOWD) a non-governmental organization (NGO) that sponsors the only American surgical mission to Niger (http://www.nigerfistula.org/).
Naked foam rubber mats, rinsed out daily with a garden hose lay flat in the sun to dry, ready for another night of urine-soaked sleep. The women are immaculate and enterprising, making beaded jewelry and learning to sew on machines donated by the International Organization for Women and Development (IOWD) a non-governmental organization (NGO) that sponsors the only American surgical mission to Niger (http://www.nigerfistula.org/). 
 The hospital is a former military installation built for quarantine in a network of single story low, flat-topped buildings connected by covered walkways and cement courtyards.
The hospital is a former military installation built for quarantine in a network of single story low, flat-topped buildings connected by covered walkways and cement courtyards.  Winding through the access road to the surgery building, women wrapped in Kinte cloth and long tunics and men in flowing robes and Tuareg turbans mill about in the universal comings and goings of people seeking and rendering healing. Outside, ubiquitous wood smoke spices the air, inside the low slung building the faint odor of disinfectant mixes with the dry heat. The operating rooms are doubled up with OR tables .
Winding through the access road to the surgery building, women wrapped in Kinte cloth and long tunics and men in flowing robes and Tuareg turbans mill about in the universal comings and goings of people seeking and rendering healing. Outside, ubiquitous wood smoke spices the air, inside the low slung building the faint odor of disinfectant mixes with the dry heat. The operating rooms are doubled up with OR tables .The fistula women are waiting to be seen, having camped out in the “fistula courtyard” for days or weeks, arriving from the remotest areas of Niger and the surrounding countries of Benin, Nigeria, Burkina Faso and Mali. For some, an entire year’s earnings fund the journey to this hospital. The surgery building has a sunken courtyard on one side, and after traversing the cool tiled hallways, you emerge on the courtyard cat walk to see dozens of women and their children living, some for months, others for years, in a “sisterhood of suffering".
 Naked foam rubber mats, rinsed out daily with a garden hose lay flat in the sun to dry, ready for another night of urine-soaked sleep. The women are immaculate and enterprising, making beaded jewelry and learning to sew on machines donated by the International Organization for Women and Development (IOWD) a non-governmental organization (NGO) that sponsors the only American surgical mission to Niger (http://www.nigerfistula.org/).
Naked foam rubber mats, rinsed out daily with a garden hose lay flat in the sun to dry, ready for another night of urine-soaked sleep. The women are immaculate and enterprising, making beaded jewelry and learning to sew on machines donated by the International Organization for Women and Development (IOWD) a non-governmental organization (NGO) that sponsors the only American surgical mission to Niger (http://www.nigerfistula.org/). 
Tenacity rules courtyard life; all hardship is greeted with determination and a smile.

Fistulas are abnormal connections between organs, most commonly between bladder and vagina, and also between rectum and vagina, urethra and vagina, bladder and uterus, and ureter and vagina. Fistulas occur rarely in industrialized countries, at a rate of less than 2%, most commonly a result of gynecologic surgery (82%) and less often due to childbirth injury (8%), radiation therapy (6%) and eroding cancers or infections (4%).
 For women in developing countries in Africa, Asia and Latin America, the odds are the inverse, with 92% of fistulas due to childbirth and the remainder (8%) caused by complications of gynecologic surgery, cancers or infections (Nigeria 1985, Ghana 1996). Fistula rates in high-incidence countries are difficult to calculate, since countries lacking the medical infrastructure of industrialized nations also lack the bureaucratic infrastructure to gather accurate statistics. Given, however, that childbirth fistula occurred during a birth that could have easily killed the mother, fistula rates are linked to maternal mortality, and therefore maternal mortality statistics, tracked by international health organizations, are a barometer of all childbearing trauma, including fistula.
For women in developing countries in Africa, Asia and Latin America, the odds are the inverse, with 92% of fistulas due to childbirth and the remainder (8%) caused by complications of gynecologic surgery, cancers or infections (Nigeria 1985, Ghana 1996). Fistula rates in high-incidence countries are difficult to calculate, since countries lacking the medical infrastructure of industrialized nations also lack the bureaucratic infrastructure to gather accurate statistics. Given, however, that childbirth fistula occurred during a birth that could have easily killed the mother, fistula rates are linked to maternal mortality, and therefore maternal mortality statistics, tracked by international health organizations, are a barometer of all childbearing trauma, including fistula.Worldwide maternal mortality rates are 430/100,000 woman, with a wide discrepancy between the US/Europe (11/100,000) and the poorer sections of Africa (1000/100,000), due primarily, if not entirely, to the lack of medical and obstetrical infrastructure. (WHO 1996). Lewis Wall, renowned author on the topic of childbirth injury, highlights a more meaningful statistic in his work, the lifetime risk of maternal death, or "LRMD", which reflects the likelihood that the mother will not survive any given pregnancy and the number of times she will likely become pregnant based on regional birth rates. Overall, the global LRMD is 1:60. In industrialized nations the likelihood is 1:1800; in North America and Europe the rates drop even further to 1:4000. In poor countries, the overall rate is 1:48 with rates as high as 1:7 per-pregnancy death risk in the poorest nations. (WHO 1996).
 Niger, one of the 1:7 LRMD nations, is a country of 12 million people medically served by 2 urologists and 10 obstetrician – gynecologists with a fecundity rate that is one of the highest on the planet, at an average of 8 children born per woman.
Niger, one of the 1:7 LRMD nations, is a country of 12 million people medically served by 2 urologists and 10 obstetrician – gynecologists with a fecundity rate that is one of the highest on the planet, at an average of 8 children born per woman. Dr. Ghaichatou, of the National Hospital Niamey, and liason to the United Nations Fistula Prevention Association. She is the first of her Tuareg family to earn a medical degree.
We arrive at our lodgings for the trip, a local hotel in the capital city of Niamey, nestled on the bank of the Niger River, a winding waterway populated from dawn to dusk with dugout canoes pushed about on poles by local gondoliers.

We set up the rooms, and begin, in this former French colony where most are illiterate speaking only the tribal language to which they were born and the “market language” of neighboring tribes, the dance of translation; English to French to Djerma to Hausa to Fula to Tamachek back to French to English as we slowly pull the stories out of this and that woman. These women do not understand the anatomy of their condition. They trust doctors implicitly and believe they have no right to question. This triad of ignorance, trust and submissiveness turns informed consent translations into farcical monologues met with stony, stoic forebearance.
Language is no barrier to the alien realization that many of these women don't know how old they are, and no fewer number blame not the lack of healthcare dollars nor the dearth of strategically located medical facilities as reasons for their damaged physical selves. For many, stillborn babies and the purgatory of living with fistula are the work of evil curses or divine punishments. For them, the standard of obstetric care taken for granted in industrialized nations is quintessentially foreign.
They tell stories of being moved from the family hut to the edge of the village, of living, suddenly and for the first time in solitude, allowed to plant seeds but not harvest, forced from buses or banished to the roof with the luggage, of husbands marrying new wives, of the sheer madness and reeking odor of urine or stool, or both, coming constantly constantly constantly in the 120 degree heat in a hut with one door and no windows,  of the urine crusted ulcerations extending from their most private areas to the tops of their feet. Even the most gregarious courtyard citizen turns shy entering this room full of strange hardware to confront the foreign prodding of these terrible, intimate questions.
of the urine crusted ulcerations extending from their most private areas to the tops of their feet. Even the most gregarious courtyard citizen turns shy entering this room full of strange hardware to confront the foreign prodding of these terrible, intimate questions.  With the interview complete, the screening examination begins. Back home, fistula patients have pyelograms, MRIs, CT scans, cystograms, and any number of consultations before they land on the operating table for the big event. Here in Niger, even a pyelogram is inordinately difficult to arrange, and second opinions take place in the operating room. Most are evaluated with cystoscopy and blue dye fill tests. To save money we use blue food coloring mixed with sterile saline.
With the interview complete, the screening examination begins. Back home, fistula patients have pyelograms, MRIs, CT scans, cystograms, and any number of consultations before they land on the operating table for the big event. Here in Niger, even a pyelogram is inordinately difficult to arrange, and second opinions take place in the operating room. Most are evaluated with cystoscopy and blue dye fill tests. To save money we use blue food coloring mixed with sterile saline.
 Some fistulas are easy to find; large holes between bladder and vagina the size of business cards. Others are more complicated, recurrent pinpoint fistulas with labrynthine and tiny caliber tracts connecting vagina to bladder, or connecting bladder to uterus to vagina through missing chunks of cervix. Yet others are cemented in by dense vaginal scarring, none more tragic than an 18 year old Tanzanian woman I met while working in East Africa last year, who had undergone 8 prior repairs after her first and only stillborn pregnancy. Once more at hospital to fix a recto-vaginal fistula sustained during the last (failed) attempt to recreate her vagina, she was to learn this time that all hope was gone, her vagina scarred shut from the trauma from the difficult birth and the many operations to close the hole. I could not bear to look in her eyes for more than a moment. She was the age of my daughter.
Some fistulas are easy to find; large holes between bladder and vagina the size of business cards. Others are more complicated, recurrent pinpoint fistulas with labrynthine and tiny caliber tracts connecting vagina to bladder, or connecting bladder to uterus to vagina through missing chunks of cervix. Yet others are cemented in by dense vaginal scarring, none more tragic than an 18 year old Tanzanian woman I met while working in East Africa last year, who had undergone 8 prior repairs after her first and only stillborn pregnancy. Once more at hospital to fix a recto-vaginal fistula sustained during the last (failed) attempt to recreate her vagina, she was to learn this time that all hope was gone, her vagina scarred shut from the trauma from the difficult birth and the many operations to close the hole. I could not bear to look in her eyes for more than a moment. She was the age of my daughter.
 of the urine crusted ulcerations extending from their most private areas to the tops of their feet. Even the most gregarious courtyard citizen turns shy entering this room full of strange hardware to confront the foreign prodding of these terrible, intimate questions.
of the urine crusted ulcerations extending from their most private areas to the tops of their feet. Even the most gregarious courtyard citizen turns shy entering this room full of strange hardware to confront the foreign prodding of these terrible, intimate questions.  With the interview complete, the screening examination begins. Back home, fistula patients have pyelograms, MRIs, CT scans, cystograms, and any number of consultations before they land on the operating table for the big event. Here in Niger, even a pyelogram is inordinately difficult to arrange, and second opinions take place in the operating room. Most are evaluated with cystoscopy and blue dye fill tests. To save money we use blue food coloring mixed with sterile saline.
With the interview complete, the screening examination begins. Back home, fistula patients have pyelograms, MRIs, CT scans, cystograms, and any number of consultations before they land on the operating table for the big event. Here in Niger, even a pyelogram is inordinately difficult to arrange, and second opinions take place in the operating room. Most are evaluated with cystoscopy and blue dye fill tests. To save money we use blue food coloring mixed with sterile saline. Some fistulas are easy to find; large holes between bladder and vagina the size of business cards. Others are more complicated, recurrent pinpoint fistulas with labrynthine and tiny caliber tracts connecting vagina to bladder, or connecting bladder to uterus to vagina through missing chunks of cervix. Yet others are cemented in by dense vaginal scarring, none more tragic than an 18 year old Tanzanian woman I met while working in East Africa last year, who had undergone 8 prior repairs after her first and only stillborn pregnancy. Once more at hospital to fix a recto-vaginal fistula sustained during the last (failed) attempt to recreate her vagina, she was to learn this time that all hope was gone, her vagina scarred shut from the trauma from the difficult birth and the many operations to close the hole. I could not bear to look in her eyes for more than a moment. She was the age of my daughter.
Some fistulas are easy to find; large holes between bladder and vagina the size of business cards. Others are more complicated, recurrent pinpoint fistulas with labrynthine and tiny caliber tracts connecting vagina to bladder, or connecting bladder to uterus to vagina through missing chunks of cervix. Yet others are cemented in by dense vaginal scarring, none more tragic than an 18 year old Tanzanian woman I met while working in East Africa last year, who had undergone 8 prior repairs after her first and only stillborn pregnancy. Once more at hospital to fix a recto-vaginal fistula sustained during the last (failed) attempt to recreate her vagina, she was to learn this time that all hope was gone, her vagina scarred shut from the trauma from the difficult birth and the many operations to close the hole. I could not bear to look in her eyes for more than a moment. She was the age of my daughter.18 years old Tanzanian woman, one stillborn baby, 8 fistula surgeries, total vaginal obliteration. Kilimanjaro Catholic Medical Center, Moshi Town, Tanzania August 2006.
Some can be fixed, some cannot. Urinary diversions, the standard of care for irreparable fistulae in wealthy nations, entail a life time of follow-up, dietary supplements and access to acute care facilities to treat the unpredictable and life-long complications of such operations. In a third world setting, these reconstructive diversions are an ethical dilemma, the safest choice of which is to simply not do them. All fistula repair surgeons and aid programs know this phenomenon of the truly doomed too well. It is the step-child of fistula work.
 Robustly funded programs offer long term lodging and occupational training (www.fistulafoundation.org).
Robustly funded programs offer long term lodging and occupational training (www.fistulafoundation.org). Dr. Clifford Wheeless, Dr. Lauri Romanzi and Dr. Gopal Badlani
second opinion evaluation, Niamey, Niger 2004
For those fortunate enough to be operable, the case lists include their names and the elaborate, multi-tribal translation of pre-op instructions is carried out.
Next morning, with two tables in each room, the OR hums with endeavor.
Next morning, with two tables in each room, the OR hums with endeavor.

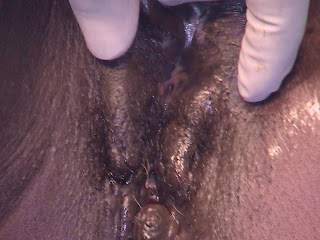
My first case on this mission was an enormous hole connecting the bladder to the uterus through a missing segment of cervix so that all the urine poured into the vagina non-stop.

Vesico-utero-cervico-vaginal fistula:
(bladder into uterus through defect in cervix into vagina) Niamey, Niger 2006
We were always prepared for a blackout, flashlights in our pockets and camping headlights around our necks to use until the generators kick into action.
Dr. Ghaichatou, Dr. Badlani and Dr. Romanzi operating by the light of a generator. Niamey, Niger 2004
It was on this second journey as a volunteer fistula surgeon to Niger that I met the woman who taught me what it truly means to expect the unexpected. She was the first patient I saw that day, 20 years old claiming never to have given birth at all, but only to have miscarried one time, 3 years ago. She had never gotten pregnant again after that. And mysteriously, about a year before making the trip to Niger, she began to leak, just a little at first, and not every day, and then slowly over months, the drip turned to a constant flow, and her world turned upside down. Her striking features highlighted by the tattooed black lips of her Fulani tribe, her eyes never left my face as she told her story to the translator. Two solid weeks it took her to walk to the capital. The American doctors had to fix her. All of her so that the leaking would stop and her fertility be restored. Her husband’s family was pressuring him to take another wife, one who could give him babies and live in his hut. Forced to exile herself to separate quarters, her world shrinking to a solitary confinement of ever increasing hardship, desperation was her sole companion.
Her story did not make any sense. She hadn’t birthed a baby, she had no fevers or infections, no surgery, no accidents or physical injury, so where was the urine coming from? I worried that she might have a congenital anomaly, literally born with faulty plumbing, one kidney and a misplaced ureter, perhaps. Sometimes these defects don’t become evident until a girl is a teenager. If so, the surgery might need to be done in stages, one surgery now, returning for the next part three months down the road when the next group of surgeons was scheduled to come to Niger. Would she be able to make it back to the capital on another 2 week walk? Or maybe there was something she wasn’t telling us. In the bush, local healers sometimes resort to harsh interventions to cure gynecologic maladies. Had she been made to sit on stones hot as coals or had rock salt inserted into her vagina to heal her infertility?
As she reclined on the examining table, the answers continued to evade me as I watched the urine drip onto the table pads, unusually pink-tinged with blood. Attempting to examine her, she flinched in pain; something rocky was in the vagina, or was it the bladder? It looked like a stone, very rare in a such young woman but not impossible. The “stone” was in the fistula hole, which was large, but the stone wouldn’t budge. Why hadn’t it passed? The hole was larger than the stone; it should have come out long ago. And why had it eroded through in the first place? Bladder stones don’t usually do that, even when they are the size of lemons. This one was the size of a small grape. An x-ray showed a bizarre calcified mass in the pelvis that was smooth and round on one end and spiky on the other. Bladder stones are usually smooth and round, like pearls. She had two kidneys; a big relief. But the puzzle of the bladder stone seemed to increase with each step of the evaluation.
Under anesthesia, we used an instrument called a cystoscope to look into the bladder were the spiky calcifications jutted out into the camera lens like spokes on a wheel. As the exploratory surgery continued, we found a fistula that connected the uterus to the bladder and the bladder to the vagina. The spiky parts of the calcification were stuck in the uterus, the smooth round part was pushing into the vagina. Exposing the defect to begin the tedious work of figuring out what went where and how to put her parts back together again, the mystery was solved. It wasn’t a stone at all; it was the balled up skeleton of a fetus. Carefully removed bone by bone, ribs the size of toothpicks and a tiny fossilized skull bore witness on the instrument table.

She had miscarried, true, but not completely, the bones stuck inside, acting like an IUD (intra-uterine device), preventing conception for all these years. And then, a year ago, the bones eroded through the wall of the uterus into the bladder and then into the vagina, causing as complicated a fistula as can be.
We restored her body, this is sure. I may never know if the same is true of her life, but I like to believe that this also is true. That she is back in her village, living in her husband’s hut, baby strapped to her back, faith in her future restored. I also like to believe that she, and all of her fistula sisters, have borne their share of hardships for one lifetime, each and every one granted a lifetime reprieve as they pass for the last time through the gate of the hospital onto the dusty road home.
It is tempting to presume that young marriage and poor nutrition cause these difficult, fistula inducing labors. To be honest, we really aren't sure about that. In Niger, for instance, there is a bimodal distribution. Fistula happens with the first baby, which in third world countries usually occurs in young women because they marry young. Or fistula occurs after several babies, often the largest birthweight, to a woman in her 30's or 40's. It is very likely more a matter of how the baby "fits" than an absolute function of maternal age. Here in the U.S., teenaged mothers abound and fistula is almost unheard of. So, is maternal age the biggest issue? Very likely not.

Fistula after the birth of her 7th child
(on bed, 14 years old) fistula after her first baby

Citizens of impoverished countries know well what most in the industrialized world have forgotten; childbearing is a life-threatening process. The harsh bonds between procreation and death live on in the romance literature of the 19th century, rife as it was with imagery of young women dying in the throws of childbirth leaving behind orphaned children to be raised by pining fathers and extended family, as did the golden-hearted but frail Melanie in "Gone with the Wind".
Here in the US the transition from home birth to hospital birth occurred over a period of 15 years between 1940 (50%) and 1955 by which time 99% of US births took place in a hospital. This shift was in no small part due to the then novel utilization of cesarean to save the life or improve the outcome of the mother, and then eventually of the baby, as the operation was made reliably safe by the combination of antibiotics, antisepsis and modern anesthesia. (http://www.nlm.nih.gov-cesarian/ Section-a brief history, National Library of Medicine).
Prior to the late 1800’s, cesarean in Europe and the US was performed primarily to rescue live infants from dead mothers. With the advent of antibiotics and safe anesthesia, the transition from post-mortem neonatal rescue to maternal rescue to optimal outcome for both mother and baby was complete by the mid-20th century, and with it a concurrent plummeting in the incidence of obstetrical fistula. J. Marion Sims, father of fistula repair, contributed his portion to this legacy of operative birthing.
J. Marion Sims using silver wire to repair fistula 1870 (National Library of Medicine)

Fistula after the birth of her 7th child
(on bed, 14 years old) fistula after her first baby

Citizens of impoverished countries know well what most in the industrialized world have forgotten; childbearing is a life-threatening process. The harsh bonds between procreation and death live on in the romance literature of the 19th century, rife as it was with imagery of young women dying in the throws of childbirth leaving behind orphaned children to be raised by pining fathers and extended family, as did the golden-hearted but frail Melanie in "Gone with the Wind".
Here in the US the transition from home birth to hospital birth occurred over a period of 15 years between 1940 (50%) and 1955 by which time 99% of US births took place in a hospital. This shift was in no small part due to the then novel utilization of cesarean to save the life or improve the outcome of the mother, and then eventually of the baby, as the operation was made reliably safe by the combination of antibiotics, antisepsis and modern anesthesia. (http://www.nlm.nih.gov-cesarian/ Section-a brief history, National Library of Medicine).
Prior to the late 1800’s, cesarean in Europe and the US was performed primarily to rescue live infants from dead mothers. With the advent of antibiotics and safe anesthesia, the transition from post-mortem neonatal rescue to maternal rescue to optimal outcome for both mother and baby was complete by the mid-20th century, and with it a concurrent plummeting in the incidence of obstetrical fistula. J. Marion Sims, father of fistula repair, contributed his portion to this legacy of operative birthing.

J. Marion Sims using silver wire to repair fistula 1870 (National Library of Medicine)

In most texts Sims is celebrated as a hero, working ceaselessly to perfect fistula repair among slaves, operating on some women dozens of times to relieve them of this horrid affliction. In other publications he is reviled as a butcher, operating on slaves without their consent and or consideration for their pain and suffering under the knife. Whichever your perspective, his pioneering surgical principles and techniques are used to this day and his discovery that silver wire sutures reduced wound infection was also introduced to the cesarean section (National Library of Medicine), facilitating the emerging technique of closing the uterus with sutures and reducing wound healing complications. His Fistula Hospital, opened in the 1850’s on New York City’s Park Avenue, was obsolete within 40 years, and was razed for the construction of the Waldorf Astoria Hotel that opened its doors in 1893.
 Yes, it was here; our own fistula hospital and our own fistula problem vanquished by the advent of safe, modern obstetrical practice so that we now live with the luxury that any given woman will most likely survive any given pregnancy and have a healthy infant to show for it. We have the (justified) luxury of criticizing our healthcare system for the medicalization of pregnancy and the over-utilization of the very procedure that reduced the incidence of obstetrical fistula to almost nothing and we have the luxury of looking abroad in wonderment at the conditions under which the majority of the world’s women continue to give birth as if obstructed labor and fistula formation are truly, fundamentally foreign. These women are not foreign; these women are us.
Yes, it was here; our own fistula hospital and our own fistula problem vanquished by the advent of safe, modern obstetrical practice so that we now live with the luxury that any given woman will most likely survive any given pregnancy and have a healthy infant to show for it. We have the (justified) luxury of criticizing our healthcare system for the medicalization of pregnancy and the over-utilization of the very procedure that reduced the incidence of obstetrical fistula to almost nothing and we have the luxury of looking abroad in wonderment at the conditions under which the majority of the world’s women continue to give birth as if obstructed labor and fistula formation are truly, fundamentally foreign. These women are not foreign; these women are us.
Mariama and Hama, two repaired fistula patients trained as patient assistants for the IOWD fistula program (http://www.nigerfistula.org/)
Reliable epidemiologic data is a phenomenon of recent history; prior to World War II, most medical data was based on case series and institutional statistics. This makes it difficult to compare the rates of fistula in Africa now as compared to 100 years ago. Or here in the US, for that matter. But there is anecdotal evidence that cesarean section was actively and successfully practiced among African tribes before European coloniization.

Successful Cesarean section performed by indigenous healers in Kahura, Uganda. As observed by R. W. Felkin in 1879. (National Library of Medicine)
Not only was cesarean section a common and established practice, it was done with analgesia and antisepsis, both achieved with the judicious use of banana wine:
“..........., nineteenth-century travelers in Africa reported instances of indigenous people successfully carrying out the procedure with their own medical practices. In 1879, for example, one British traveller, R.W. Felkin, witnessed cesarean section performed by Ugandans. The healer used banana wine to semi-intoxicate the woman and to cleanse his hands and her abdomen prior to surgery. He used a midline incision and applied cautery to minimize hemorrhaging. He massaged the uterus to make it contract but did not suture it; the abdominal wound was pinned with iron needles and dressed with a paste prepared from roots. The patient recovered well, and Felkin concluded that this technique was well-developed and had clearly been employed for a long time. Similar reports come from Rwanda, where botanical preparations were also used to anesthetize the patient and promote wound healing.”(National Library of Medicine, nlm.nih.gov-Cesarian section)
Lister, a British surgeon and the “father of antisepsis”, promoted carbolic acid as a method by which infection’s impact on wound healing would be reduced starting in the mid-1860’s at a time when cesarian was done only to rescue yet living newborns from dead mothers (aka post-mortem neonatal rescue) And yet, for years if not decades prior, African healers were performing cesareans on live women to deliver live babies accomplished with sedation and antisepsis, not to mention reportedly good survival rates. What happened to these skilled African surgeons? Under what circumstances were these tribal cesareans performed, and how successful were they? Why did their obstetrical talents fade to a remote wood-block print in a national archive? Why are we not reading about their skills in our obstetrical history books? In a country that today as such a dearth of obstetrical care access, it is distressing to learn that 100 years ago the talent and skill to perform fistula-sparing cesarean were in Africa well before colonization. We leave these compelling questions for the medical historians and anthropologists.
Even today, epidemiologic data remains elusive throughout most of sub-Saharan Africa. Hospital-based data puts the rates in the ballpark of 350/100,000 births (Nigeria, 1985) and in some regions anecdotal estimates are much higher. On my travels in West and East Africa, the related morbidities of the obstructed labor injury complex, first described by Arrowsmith, Hamlin and Wall, are everywhere. Some women are repaired of fistula, but the scarred, sphincterless urethra results in urinary incontinence so profound that the patient's life is not improved at all. Symphyseal separation and peroneal nerve neuropraxia (foot drop) are evidenced by the waddling step, the slapping foot, and the walking stick.

Women return to clinic still frantic with looming spousal abandonment, the vaginal vault so scarred that coitus is impossible, or the uterus so damaged that menses and fertility are never regained. The repaired anal sphincter is still too weak to prevent fecal soiling, or the strictured urethra so narrow that obstructive uropathy and urinary retention preclude a return to village life. Fistula has its bedfellows, each devastating. (Arrowsmith S, Hamlin EC, Wall LL. Obstructed labor injury complex: obstetric fistula formation and the multifaceted morbidity of maternal birth trauma in the developing world. Obstet Gynecol Surv. 1995;51:568-574.)
Fistula repair programs exist here and there, some decades old, some newly minted, some government sponsored, others parochial or secular non-governmental organizations, or the efforts of solo volunteers individually augmenting the local medical staff wherever their availability meets the need. Resources vary widely and success rates are cloaked in mystery. The sheer athleticism of providing surgical care in a third world setting makes even basic data collection an exhausting chore.
The Cadillac of fistula repair centers is in Addis Ababa, Ethiopia, founded in 1959 by Australian gynecologist Dr. Catherine Hamlin (http://www.fistulafoundation.org/). This East African facility is the second hospital dedicated to fistula repair in the world after J. Marion Sims former Park Avenue hospital. Colleagues tell me of clean sheets on every bed, running water in the wards, generous supplies, specially trained staff, occupational therapy and long term facilities for those who, for various reasons, do not return to their villages. More often than not, if you read about fistula repair in a lay publication, it is Dr. Hamlin’s program. A few months ago I had the privilege of talking with two Ethiopian colleagues who work with her in Addis. Gushing with admiration, I commented on how very proud they must be of the center’s reputation and how wonderful to be available to women year round in a dedicated facility. With a quizzical glance, as if I were a bit nutty, the senior surgeon responded gently; “I will be proud when the hospital is no longer needed and is replaced by a luxury hotel”.